概要
Limiting Dilution Analysis (LDA) has been applied to the in vitro quantitation of hematopoietic stem cells (HSCs) using assays such as the long term culture-initiating cell (LTC-IC) assay (Conneally et al.) and the cobblestone area forming cell (CAFC) assay (Wang et al.). Limiting dilution protocols have also been adapted to allow the quantitation of human and mouse HSCs with the capacity to produce mature cells of all hematopoietic lineages in vivo, in competitive repopulating unit (CRU) (Ploemacher et al.; Szilvassy et al.) and SCID repopulating cell (SRC) assays (Dick et al.).
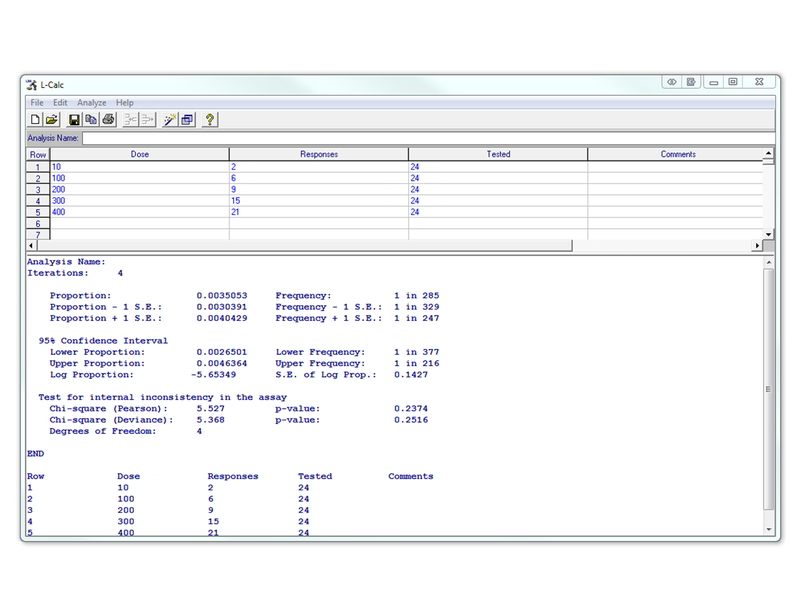
L-Calc™ will assist you in analyzing the results of your LDA. For each experiment, values corresponding to dose (i.e. cells per well); total number of positive responses obtained per dose; and total number of replicates tested (i.e. total number of wells used per cell dose) are entered. From these data, the frequency of cells within a given cell population capable of a defined response is determined. L-Calc™ can also be used as a guide to assess differences between paired sets of LDAs. A statistician should be consulted to perform the appropriate comparison.
Free Software Download Available: lcsetup.exe
Suitable for use with Microsoft® Windows.
Please note we no longer provide support or updates for L-Calc software.
L-Calc™ will assist you in analyzing the results of your LDA. For each experiment, values corresponding to dose (i.e. cells per well); total number of positive responses obtained per dose; and total number of replicates tested (i.e. total number of wells used per cell dose) are entered. From these data, the frequency of cells within a given cell population capable of a defined response is determined. L-Calc™ can also be used as a guide to assess differences between paired sets of LDAs. A statistician should be consulted to perform the appropriate comparison.
Free Software Download Available: lcsetup.exe
Suitable for use with Microsoft® Windows.
Please note we no longer provide support or updates for L-Calc software.
技术资料
数据及文献
Publications (18)
Stem cells (Dayton, Ohio) 2019 jul
p53-TP53-Induced Glycolysis Regulator Mediated Glycolytic Suppression Attenuates DNA Damage and Genomic Instability in Fanconi Anemia Hematopoietic Stem Cells.
Abstract
Abstract
Emerging evidence has shown that resting quiescent hematopoietic stem cells (HSCs) prefer to utilize anaerobic glycolysis rather than mitochondrial respiration for energy production. Compelling evidence has also revealed that altered metabolic energetics in HSCs underlies the onset of certain blood diseases; however, the mechanisms responsible for energetic reprogramming remain elusive. We recently found that Fanconi anemia (FA) HSCs in their resting state are more dependent on mitochondrial respiration for energy metabolism than on glycolysis. In the present study, we investigated the role of deficient glycolysis in FA HSC maintenance. We observed significantly reduced glucose consumption, lactate production, and ATP production in HSCs but not in the less primitive multipotent progenitors or restricted hematopoietic progenitors of Fanca-/- and Fancc-/- mice compared with that of wild-type mice, which was associated with an overactivated p53 and TP53-induced glycolysis regulator, the TIGAR-mediated metabolic axis. We utilized Fanca-/- HSCs deficient for p53 to show that the p53-TIGAR axis suppressed glycolysis in FA HSCs, leading to enhanced pentose phosphate pathway and cellular antioxidant function and, consequently, reduced DNA damage and attenuated HSC exhaustion. Furthermore, by using Fanca-/- HSCs carrying the separation-of-function mutant p53R172P transgene that selectively impairs the p53 function in apoptosis but not cell-cycle control, we demonstrated that the cell-cycle function of p53 was not required for glycolytic suppression in FA HSCs. Finally, ectopic expression of the glycolytic rate-limiting enzyme PFKFB3 specifically antagonized p53-TIGAR-mediated metabolic reprogramming in FA HSCs. Together, our results suggest that p53-TIGAR metabolic axis-mediated glycolytic suppression may play a compensatory role in attenuating DNA damage and proliferative exhaustion in FA HSCs. Stem Cells 2019;37:937-947.
Aging cell 2019 dec
Metformin blunts muscle hypertrophy in response to progressive resistance exercise training in older adults: A randomized, double-blind, placebo-controlled, multicenter trial: The MASTERS trial.
Abstract
Abstract
Progressive resistance exercise training (PRT) is the most effective known intervention for combating aging skeletal muscle atrophy. However, the hypertrophic response to PRT is variable, and this may be due to muscle inflammation susceptibility. Metformin reduces inflammation, so we hypothesized that metformin would augment the muscle response to PRT in healthy women and men aged 65 and older. In a randomized, double-blind trial, participants received 1,700 mg/day metformin (N = 46) or placebo (N = 48) throughout the study, and all subjects performed 14 weeks of supervised PRT. Although responses to PRT varied, placebo gained more lean body mass (p = .003) and thigh muscle mass (p {\textless} .001) than metformin. CT scan showed that increases in thigh muscle area (p = .005) and density (p = .020) were greater in placebo versus metformin. There was a trend for blunted strength gains in metformin that did not reach statistical significance. Analyses of vastus lateralis muscle biopsies showed that metformin did not affect fiber hypertrophy, or increases in satellite cell or macrophage abundance with PRT. However, placebo had decreased type I fiber percentage while metformin did not (p = .007). Metformin led to an increase in AMPK signaling, and a trend for blunted increases in mTORC1 signaling in response to PRT. These results underscore the benefits of PRT in older adults, but metformin negatively impacts the hypertrophic response to resistance training in healthy older individuals. ClinicalTrials.gov Identifier: NCT02308228.
Blood 2011 JUL
Crebbp haploinsufficiency in mice alters the bone marrow microenvironment, leading to loss of stem cells and excessive myelopoiesis.
Abstract
Abstract
CREB-binding protein (CREBBP) is important for the cell-autonomous regulation of hematopoiesis, including the stem cell compartment. In the present study, we show that CREBBP plays an equally pivotal role in microenvironment-mediated regulation of hematopoiesis. We found that the BM microenvironment of Crebbp(+/-) mice was unable to properly maintain the immature stem cell and progenitor cell pools. Instead, it stimulates myeloid differentiation, which progresses into a myeloproliferation phenotype. Alterations in the BM microenvironment resulting from haploinsufficiency of Crebbp included a marked decrease in trabecular bone that was predominantly caused by increased osteoclastogenesis. Although CFU-fibroblast (CFU-F) and total osteoblast numbers were decreased, the bone formation rate was similar to that found in wild-type mice. At the molecular level, we found that the known hematopoietic modulators matrix metallopeptidase-9 (MMP9) and kit ligand (KITL) were decreased with heterozygous levels of Crebbp. Lastly, potentially important regulatory proteins, endothelial cell adhesion molecule 1 (ESAM1) and cadherin 5 (CDH5), were increased on Crebbp(+/-) endothelial cells. Our findings reveal that a full dose of Crebbp is essential in the BM microenvironment to maintain proper hematopoiesis and to prevent excessive myeloproliferation.
Blood 2011 JAN
Angiopoietin-like protein 3 supports the activity of hematopoietic stem cells in the bone marrow niche.
Abstract
Abstract
The physiologic roles of angiopoietin-like proteins (Angptls) in the hematopoietic system remain unknown. Here we show that hematopoietic stem cells (HSCs) in Angptl3-null mice are decreased in number and quiescence. HSCs transplanted into Angptl3-null recipient mice exhibited impaired repopulation. Bone marrow sinusoidal endothelial cells express high levels of Angptl3 and are adjacent to HSCs. Importantly, bone marrow stromal cells or endothelium deficient in Angptl3 have a significantly decreased ability to support the expansion of repopulating HSCs. Angptl3 represses the expression of the transcription factor Ikaros, whose unregulated overexpression diminishes the repopulation activity of HSCs. Angptl3, as an extrinsic factor, thus supports the stemness of HSCs in the bone marrow niche.
Blood 2010 MAR
Slug deficiency enhances self-renewal of hematopoietic stem cells during hematopoietic regeneration.
Abstract
Abstract
Both extrinsic and intrinsic mechanisms tightly govern hematopoietic stem cell (HSC) decisions of self-renewal and differentiation. However, transcription factors that can selectively regulate HSC self-renewal division after stress remain to be identified. Slug is an evolutionarily conserved zinc-finger transcription factor that is highly expressed in primitive hematopoietic cells and is critical for the radioprotection of these key cells. We studied the effect of Slug in the regulation of HSCs in Slug-deficient mice under normal and stress conditions using serial functional assays. Here, we show that Slug deficiency does not disturb hematopoiesis or alter HSC homeostasis and differentiation in bone marrow but increases the numbers of primitive hematopoietic cells in the extramedullary spleen site. Deletion of Slug enhances HSC repopulating potential but not its homing and differentiation ability. Furthermore, Slug deficiency increases HSC proliferation and repopulating potential in vivo after myelosuppression and accelerates HSC expansion during in vitro culture. Therefore, we propose that Slug is essential for controlling the transition of HSCs from relative quiescence under steady-state condition to rapid proliferation under stress conditions. Our data suggest that inhibition of Slug in HSCs may present a novel strategy for accelerating hematopoietic recovery, thus providing therapeutic benefits for patients after clinical myelosuppressive treatment.
Blood 2010 DEC
Progenitor cell dose determines the pace and completeness of engraftment in a xenograft model for cord blood transplantation.
Abstract
Abstract
Two critical concerns in clinical cord blood transplantation are the initial time to engraftment and the subsequent restoration of immune function. These studies measured the impact of progenitor cell dose on both the pace and strength of hematopoietic reconstitution by transplanting nonobese diabetic/severe combined immunodeficiency/interleukin-2 receptor-gamma-null (NSγ) mice with lineage-depleted aldehyde dehydrogenase-bright CD34(+) human cord blood progenitors. The progress of each transplant was monitored over an extended time course by repeatedly analyzing the peripheral blood for human hematopoietic cells. In vivo human hematopoietic development was complete. After long-term transplantation assays (≥ 19 weeks), human T-cell development was documented within multiple tissues in 16 of 32 NSγ mice. Human T-cell differentiation was active within NSγ thymuses, as documented by the presence of CD4(+) CD8(+) T-cell progenitors as well as T-cell receptor excision circles. It is important to note that although myeloid and B-cell engraftment was detected as early as 4 weeks after transplantation, human T-cell development was exclusively late onset. High progenitor cell doses were associated with a robust human hematopoietic chimerism that accelerated both initial time to engraftment and subsequent T-cell development. At lower progenitor cell doses, the chimerism was weak and the human hematopoietic lineage development was frequently incomplete.

 网站首页
网站首页